

One of the world’s largest global health initiatives (GHI), vaccine alliance Gavi, started in a UNICEF basement with a staff of five people. Nearly 25 years later, Gavi has grown into one of the most influential players on the global health stage, driving progress on key global health challenges.
Yet several experts on global health finance contend that large non-UN multilateral health organizations like Gavi and Global Fund need to gradually turn more of their functions to countries – and devolve into less costly, more country-based institutions.
The Geneva Graduate Institute hosted a frank conversation on the future of GHIs alongside the 77th World Health Assembly and Gavi and the Global Fund’s soon-to-be launched “replenishment” campaigns.
GHIs have been accused of fragmenting global health efforts, challenging the authority of the World Health Organization (WHO) and privileging donor and private-sector interests while evading accountability.
Remarkable achievement but little transparency
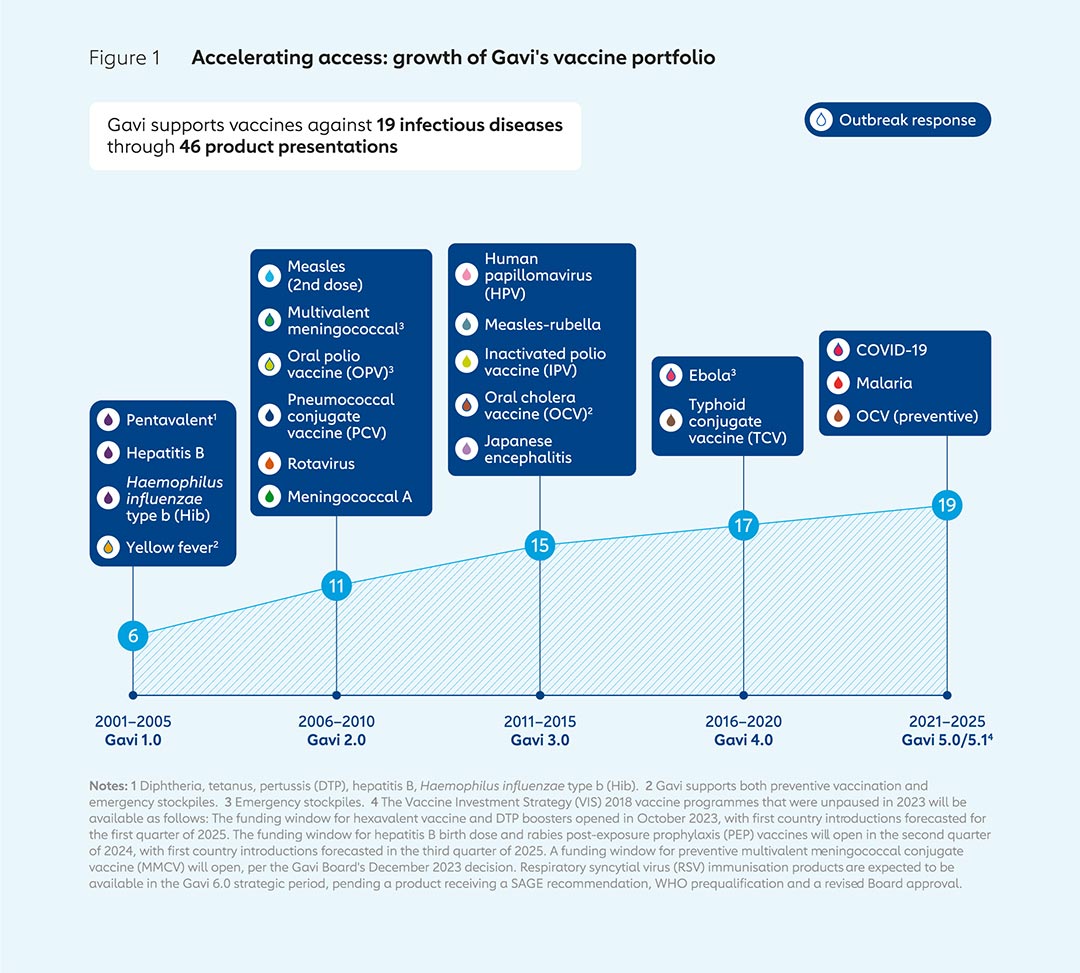
Gavi and the Global Fund, the largest of these GHIs, “really challenged the established ways of working through the World Health Organization, of the traditional multilateral system,” said Professor Katerini Storeng from the University of Oslo’s Centre for Development and the Environment.
“They did so specifically by giving additional seats at the table to commercial companies, civil society organizations and to philanthropic foundations,” she said.
This novel private-public partnership “fundamentally reshaped global health governance around private sector principles like innovation, technological solutions, and the protection of intellectual property rights,” said Storeng.
Not only did GHIs introduce a private sector mentality to global health financing, but their model was “quickly embraced,” according to Storeng. One of the most recent examples of the application of the model was with the Gavi-directed global COVAX campaign during the COVID-19 pandemic.
However, Storeng noted that the pandemic reignited old debates, including around how these partnerships are dominated by a handful of powerful GHIs and “the apparent conflict of interest arising from the inclusion of for profit actors into formal institutions of global health governance.”
Experts have reiterated calls for better coordination between global health partnerships and for their greater alignment with national health plans and priorities. While others have rejected such calls for incremental change asking for more radical reform or even present organizations to be together.
Three main developments have completely altered the GHI landscape, namely a shift towards bureaucratization, expanded mandates, and shifting cooperation with other partners, according to Antoine de Bengy Puyvallée, a PhD Fellow at University of Oslo’s Centre for Development and the Environment.
GHIs have moved from being coalitions to completely separate organizations with increasingly broader missions. Furthermore, Puyvallée notes that budgets have grown “astronomically,” tripling from 2005 to 2015, meaning more staff and a greater physical footprint in the global health hotspot of Geneva.
Their CEOs are now public figures, and their missions now encompass a wide range of goals beyond their original mandates. Gavi, for example, has expanded its activities to include diagnostics not just vaccinations, noted Puyvallée.
“You see this journey from vaccinating children to strengthening health systems,” he said. The problem with this growth, however, is the lack of accountability. “Are the boards in control?”
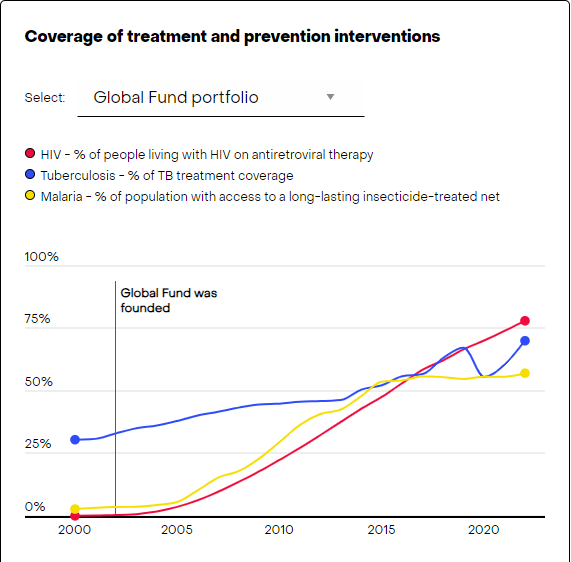
“Moving forward it is wise to think of new ways to keep these partnerships accountable together – a coordination mechanism that goes beyond the traditional ways of being governed by their own boards – otherwise it’s very difficult for accountability,” concluded Puyvallée.
The Global Fund says that its programs have saved 59 million lives since 2002, making significant strides in reducing deaths from HIV, TB, and malaria. Its 2022 numbers show that HIV prevention services increased by 22% compared to 2021, and the number of people diagnosed and treated for TB increased by 26%.
Calls for transparency and accountability
Making these GHIs more transparent and accountable requires five key strategic shifts, according to Mercy Mwangangi, director of Health Systems Strengthening at AMREF Health Africa, and former co-chair of the Future of Global Health Initiatives.
These are: investing in primary healthcare, play a catalytic role in strengthening domestic resources, champion for equity when mandates are expanded, achieve strategic and operational coherence, and mobilize research and development.
These five shifts were identified by the Lusaka Agenda, an international and multi-stakeholder dialogue.
Mwangangi noted that the Global Fund and Gavi now have a joint partnership around malaria vaccine and health systems strengthening, but asked: “How do we ensure that these shifts lead to in-country implementation?”
She stressed the need to keep country-level changes and implementation at the forefront through strengthened partnerships “otherwise we’ll just keep going round and round in circles.”
Mwangangi also called for the widespread adoption of the Lusaka Agenda to ensure that countries have a bigger voice and agency in the GHI ecosystem, but was optimistic about GHI reform.
“The boards have actually taken ownership of this issue and have shown interest in the Lusaka Agenda,” she added.
However, Anders Nordstrom, a founding member of the Global Fund and former WHO Director General, argued that there is much to do to improve the transparency and accountability of GHIs.
“The board of the Global Fund should actually discuss the yearly results report. I mean, for business, that’s one of the core responsibilities of a board. You should approve the annual report.
“That is not happening with the Global Fund. You approve the annual financial statement. There’s no link in between where you spent the money and the annual report. So in their annual report, there are no financial figures. And the annual report is very, very good, actually, but the board is not including it in discussion.”
Nordstrom went on to explain that if the boards do this, they could then “discuss the efficiency and effectiveness of the use of the money.”
Self reliance and political responsibility

For countries historically on the receiving end of support from GHIs, there has been a growing concern about health systems independence.
“Why should initiatives like Gavi buy our basic commodities?” asked Professor Justice Nonvignon, head of Health Economics Unit at Africa CDC and part of the University of Ghana’s Health Economics department.
Nonvignon argued that countries like Ghana need to domestically fund more robust health efforts, and wean themselves off of dependency.
Instead of a reliance on GHIs for basic needs, countries should provide domestic funds to buy these commodities, which range from syringes to drugs and vaccines, argued Nonvignon.
These countries have the means to channel funding to health if they choose to prioritize it, added Nordstrom.
“There are plenty of resources,” he said, noting that while working in Sierra Leone he was told that “it’s quite a rich country, plenty of diamonds and rare minerals. But where is that money?”
Mwangangi, who works closely with the Kenyan government, shared that it is incredibly difficult for African nations to transition off this dependency.
“As long as there’s no sunset clause, as long as there’s no forced transition plans and more forced graduation plans, the Ministry of Finance will not move,” she said.
Reducing reliance on aid, while difficult in the short-term, is a must, said Nonvignon, because it increases a country’s resilience and ability to act fast in an emergency.
“Cholera is devastating huge populations across central and southern Africa. Where is the time to send a proposal to a fund based in Washington DC or in Geneva?” asked Nonvignon.
“Why is the Global Fund situated in Geneva and not in Nairobi? Why is the Global Fund not in Addis Ababa instead of Geneva? Because it gives a tremendous amount of power.”
In response, Nordstrom noted that much of the global health initiative ecosystem is highly political and “the power is not with the secretariat, it’s not with the directors, it’s with the governments that provide the funding.”
“I’m worried that we’ve got the epidemiology wrong… the majority of people are losing their lives to non-communicable diseases. And the global health partnerships and community are not addressing that at all,” he said, adding that the GHI community has also failed to include the effects of a changing climate.
Sunsetting GHIs by 2030?
Nonvignon proposed sunsetting GHIs by 2030, because they have a “fundamental design flaw” in that they were established with no end date in mind.
“We are beginning to see an increase in the desire of our member states [of Africa CDC] to invest money…we need to push countries to take more responsibility.”
He noted that the pandemic prompted countries to increase their domestic spending on health, which will increase their long-term financial sustainability but cautioning that reducing aid from GHIs should not mean that philanthropies fill in the gap.
African countries must “step up,” through regional groupings such as the African Union, he added.
Putting the “onus” on countries themselves will help build global health independence – but countries need to domestically fund their own health efforts, said Mwangangi.
While a termination date for donors may seem drastic, it will at least create the space for conversation about the sustainability of GHIs, and the ability of countries to find their health financing footing.
Image Credits: S. Samantaroy/HPW, GAVI, The Global Fund, Africa CDC .
Combat the infodemic in health information and support health policy reporting from the global South. Our growing network of journalists in Africa, Asia, Geneva and New York connect the dots between regional realities and the big global debates, with evidence-based, open access news and analysis. To make a personal or organisational contribution click here on PayPal.
link





